HIV and Older People
Key Points
- As of 2022, about 54% of people with HIV in the United States were aged 50 and older.
- HIV risk factors are similar for people of all ages, but older people may be less likely to get tested for HIV.
- Treatment with HIV medicines is recommended for everyone with HIV. The best treatment regimen depends on each person’s health needs, daily routine, other medicines, and personal preferences.
- Older people may have unique factors to consider when planning HIV treatment, including other health conditions like cardiovascular disease, diabetes, kidney disease, and cancer.
Does HIV affect older people?
Yes. Because modern HIV medicines (called antiretroviral therapy or ART) are highly effective, many people with HIV live long, healthy lives. According to the Centers for Disease Control and Prevention (CDC), more than half of people with HIV in the United States were at least 50 years old. This means more people are living–and therefore aging–with HIV.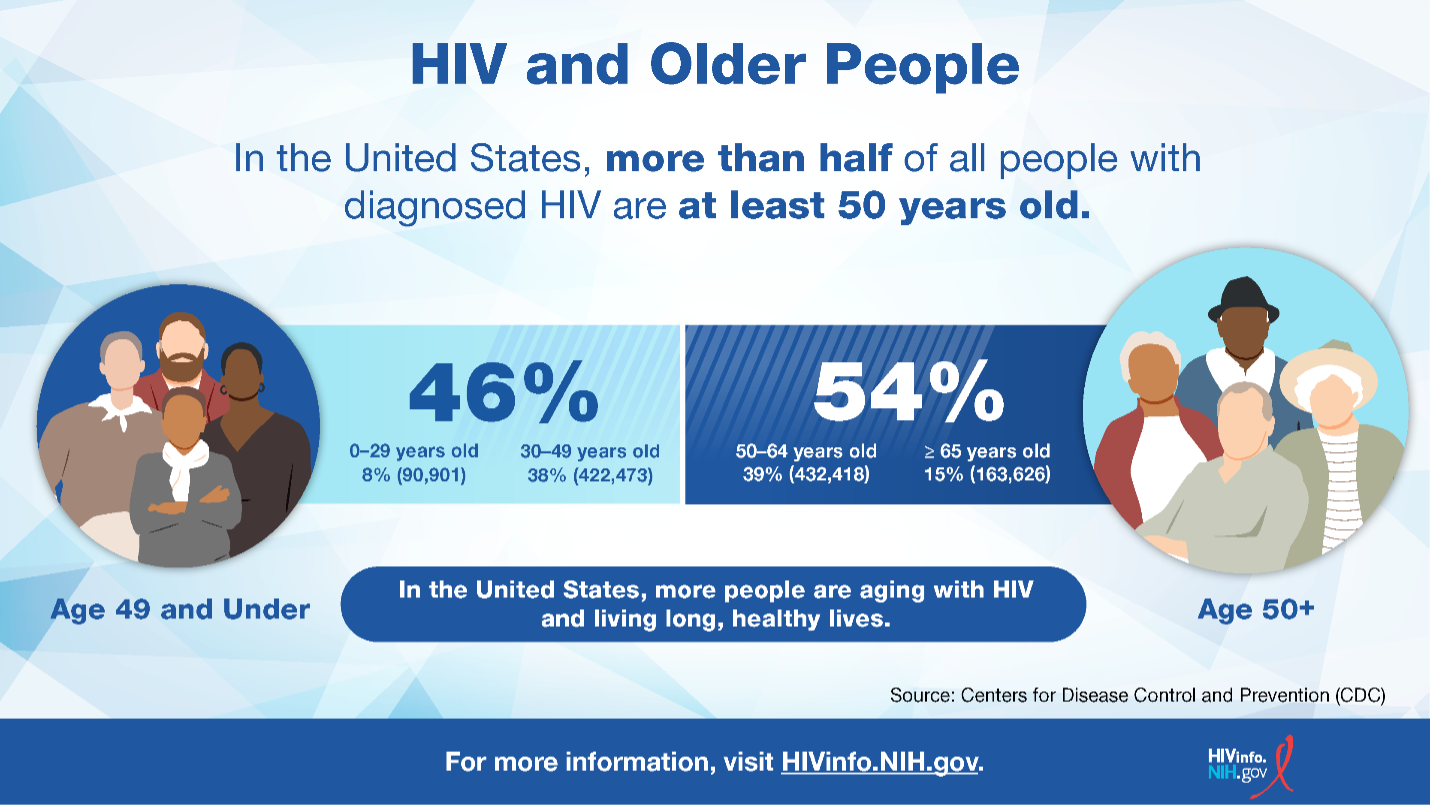
In 2022, people aged 50 years and older made up 16% of all new HIV diagnoses in the United States, less than half the share among people aged 20 to 29.
Do older people have the same risk factors for HIV as younger people?
Many HIV risk factors are similar for people of all ages. It is important for everyone, including older people, to have knowledge, understanding, and awareness of their HIV risk factors.
HIV is spread mainly by:
- Having anal or vaginal sex with someone who has a detectable amount of HIV in the blood (meaning they are not virally suppressed) without using a condom or other barrier method and not taking medicines to prevent HIV (pre-exposure prophylaxis or PrEP).
Fact: A person living with HIV who is on treatment and maintains an undetectable viral load (meaning they are virally suppressed) has zero risk of transmitting HIV to their sexual partners. This concept is called Undetectable = Untransmittable or U=U.
- Sharing injection drug equipment (works or cookers) such as needles and syringes with someone who has HIV. Use new equipment for each injection and do not share needles and syringes with other people.
Some age‑related changes may increase the likelihood of HIV transmission. For example, vaginal dryness and thinning of the vaginal lining after menopause can make the tissue more fragile. Fragile tissue may be more likely to tear during sex, which can increase the chance of HIV entering the body.
Older people may also be less likely to use condoms during sex because they are less concerned about pregnancy. Because of these factors, it can be helpful to talk with a health care provider about your HIV risk factors and ways to reduce them.
Should older people get tested for HIV?
The CDC recommends that everyone 13 to 64 years old get tested for HIV at least once as part of routine health care. People with certain HIV risk factors should get tested at least once per year. A health care provider may recommend HIV testing for an adult older than 64 if they have certain risk factors.
For several reasons, older people are less likely to get tested for HIV:
- Many people believe older adults are unlikely to acquire HIV. For this reason, health care providers may not recommend testing, and older adults may not request it.
- Some older people may be embarrassed or afraid to be tested for HIV.
- Some HIV symptoms may be mistaken for those of other age-related conditions. As a result, HIV testing may be overlooked.
Because these reasons can delay diagnosis, HIV is more likely to be diagnosed at an advanced stage in many older people. For example, the CDC reported that people aged 65 years and older made up more than one-third (33.9%) of all stage 3 HIV (AIDS) diagnoses in 2023.
A late-stage HIV diagnosis can increase the chances of damage to the immune system. A delayed HIV diagnosis delays treatment with HIV medicines. Studies have shown that early treatment is one of the most effective ways to control HIV and prevent other serious illnesses.
Ask a health care provider about the benefits of HIV testing. Use these questions from Health.gov to start the conversation: HIV Testing: Questions for the Doctor.
Are there any issues that affect HIV treatment in older people?
Treatment with HIV medicines is recommended for everyone with HIV. As for anyone with HIV, the choice of an HIV treatment regimen for an older person is based on their individual needs, daily routine, other medicines, and personal preferences.
However, HIV treatment can be more complicated for older people for reasons like:
- Comorbidities such as heart disease or cancer are more common in older people and require additional medical care.
- Side effects from HIV medicines may be more troublesome in older people with HIV.
- Medicines for other conditions can lead to drug interactions with HIV medicines that may cause unpleasant side effects.
- Drug resistance is more likely to develop over time, which can limit HIV treatment options.
- Age-related memory loss or cognitive impairment can make it harder to stick to an HIV treatment regimen.
Because older people often have other health conditions, routine screening for age-related health concerns may be necessary.
This fact sheet is based on information from the following sources:
From CDC:
- HIV Surveillance Report, 2021
- HIV Surveillance Report, 2022
- HIV Surveillance Supplemental Report, 2022
- HIV Testing
From the HIV Clinical Practice Guidelines at Clinicalinfo.HIV.gov:
- Guidelines for the Use of Antiretroviral Agents in Adults and Adolescents With HIV:
From the NIH National Institute on Aging:
Also see the HIV Source collection of HIV information and resources.
