HIV and Gay and Bisexual Men
*NOTE: Males who do not identify as gay or bisexual but engage in male-to-male sexual contact are included in this group.
Key Points
- In the United States, gay and bisexual men are the population group most affected by HIV.
- HIV testing is recommended for all sexually active gay and bisexual men at least once a year. However, some sexually active gay and bisexual men may benefit from getting tested as often as every 3 to 6 months.
- Gay and bisexual men who may be exposed to HIV should consider pre-exposure prophylaxis (PrEP) to reduce their chances of HIV infection. PrEP can reduce the risk of HIV from sex by as much as 99% when taken exactly as prescribed.
How does HIV affect gay and bisexual men?
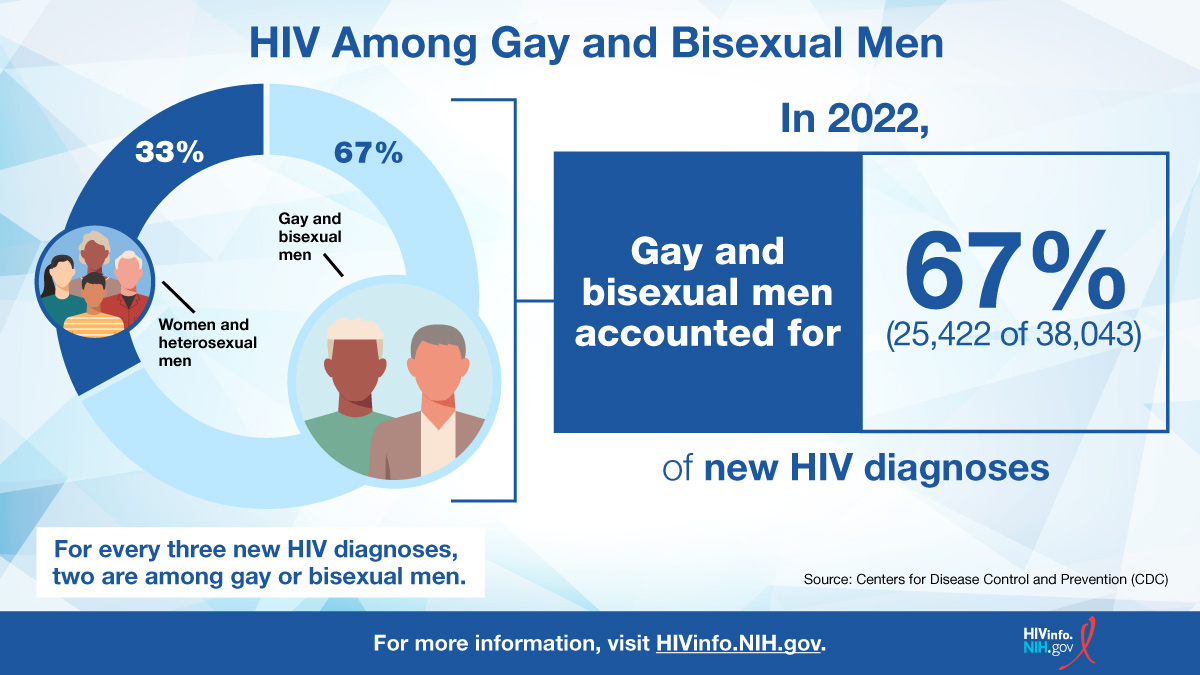
In the United States, gay and bisexual men are the population most affected by HIV. According to the Centers for Disease Control and Prevention (CDC), in 2022, adolescent and adult gay, bisexual, and other men who reported male-to-male sexual contact accounted for 67% of the new HIV diagnoses in the United States and dependent areas.
In addition, gay and bisexual men may be less likely to start or continue HIV treatment. For example, only about 68% of all gay and bisexual men with HIV were virally suppressed in 2022. When a person is not virally suppressed, it is harder to stay healthy and can increase the chance of passing HIV to others.
What factors put gay and bisexual men at risk for HIV infection?
Factors that put gay and bisexual men at risk for HIV infection:
- Sexual contact without using HIV prevention strategies. Male‑to‑male sexual contact without using condoms or taking medicines to prevent HIV. According to the CDC, receptive anal sex carries the highest risk of HIV transmission among all types of sex. The risk of transmission is about 13 times greater with receptive anal sex than with insertive anal sex.
- Homophobia, stigma, and discrimination. Negative attitudes about homosexuality may discourage gay and bisexual men from getting tested for HIV and finding health care to prevent and treat HIV.
What steps can gay and bisexual men take to prevent HIV infection?
Men can take the following steps to reduce the likelihood of HIV infection:
Know the risks.
The risk of HIV transmission varies by sexual activity, with oral sex posing much lower risk than vaginal or anal sex. However, it is hard to know the exact risk because a lot of people who have oral sex also have anal or vaginal sex. Other sexually transmitted infections (STIs), such as syphilis, herpes, gonorrhea, and chlamydia, can be transmitted during oral sex.
Make sure partners with HIV are receiving treatment.
HIV medicines can lower the amount of virus in the body to an undetectable level when taken as prescribed. People with an undetectable viral load have effectively no risk of transmitting HIV through sex, a concept known as Undetectable = Untransmittable (or U=U).
Limit the number of sex partners.
Multiple or concurrent sex partners can increase exposure to HIV and STIs. STIs can create inflammation or open sores that make it easier for HIV to enter the body.
Use condoms correctly with every sexual encounter.
Condoms can reduce the chances of transmitting HIV or other STIs when used correctly. For example, condoms are estimated to reduce HIV risk by as much as 80%. Read this CDC fact sheet on how to use a condom.
Consider HIV prophylaxis.
Pre-exposure prophylaxis (PrEP) is HIV medicine taken before a potential exposure to prevent infection. PrEP is best for people who are more likely to be exposed to HIV. To learn more, read the HIVinfo fact sheet on Pre-Exposure Prophylaxis (PrEP).
In contrast, post-exposure prophylaxis (PEP) is HIV medicine taken after a possible exposure to HIV to help prevent infection. PEP is for emergencies and does not replace PrEP or other prevention methods. To learn more, read the HIVinfo fact sheet on Post-Exposure Prophylaxis (PEP).
Get tested for HIV.
Regular HIV testing helps people make informed decisions about preventing or treating HIV. Identifying HIV early supports effective treatment and lowers the chance of passing HIV to others.
How often is HIV testing recommended for gay and bisexual men?
The CDC recommends that all men who have male-to-male sexual contact get tested for HIV at least once a year. However, some sexually active men may benefit from getting tested more often (every 3 to 6 months).
A health care provider can help determine an appropriate HIV testing schedule based on each person’s HIV risk factors. Visit the Let’s Stop HIV Together webpage to learn more about HIV testing and to find a local testing location.
This fact sheet is based on information from the following sources:
From CDC:
- HIV Surveillance Report, 2022
- HIV and Gay and Bisexual Men
- Preventing HIV With PrEP
- Preventing HIV With PEP
- Preventing HIV
- HIV Risk: About the Data
- Safer Sex 101 for HIV (PDF)
Also see the HIV Source collection of HIV links and resources.