HIV and Children
Key Points
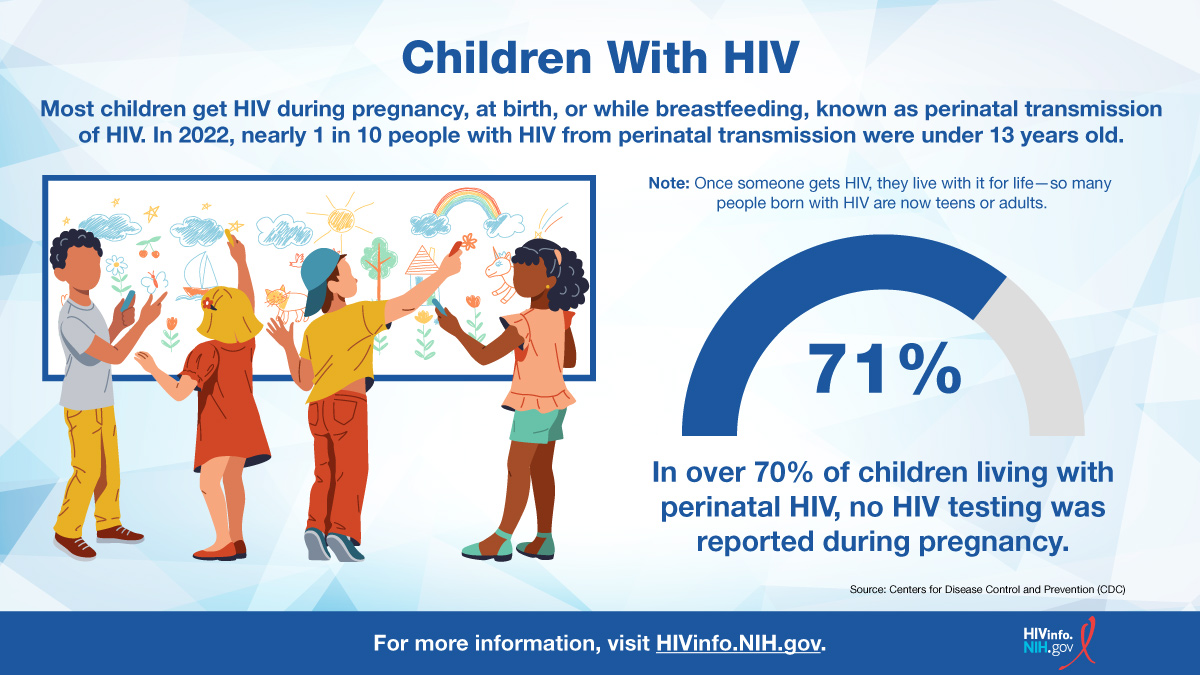
- HIV can be passed on to children during pregnancy, at childbirth, or while breastfeeding. This is called perinatal transmission. In the United States, perinatal transmission is very rare, but it is the most common way children aged under 13 years get HIV.
- Early HIV diagnosis during pregnancy and the effective use of modern HIV medicines have reduced the likelihood of perinatal transmission to less than 1%. In 2021, only 21 infants in the United States acquired HIV through perinatal transmission.
- Several factors affect HIV treatment in children, including a child’s age, weight, and overall health.
- HIV medication adherence can be difficult for children. For example, a child may refuse to take HIV medicine because it tastes unpleasant.
Does HIV affect children?
Yes, HIV affects children. According to the Centers for Disease Control and Prevention (CDC), 170 children younger than 13 years old were diagnosed with HIV in the United States and Puerto Rico from 2018 to 2021.
With modern HIV treatment, people with HIV live long, healthy lives. As of 2022, nearly 13,000 youth and adults in the United States were living with HIV acquired through perinatal transmission. People who acquired HIV at birth or shortly after are referred to as lifetime survivors or Dandelions.
How do most children get HIV?
HIV can pass to a baby during pregnancy, childbirth, or breastfeeding. In the United States, while very rare, it is the most common way children under 13 get HIV. Perinatal transmission of HIV is sometimes called mother-to-child or vertical transmission.
When taken as prescribed, HIV medicines (called antiretroviral therapy or ART) can lower the amount of HIV in the blood to an undetectable level, a state called viral suppression. When HIV stays suppressed during pregnancy, any type of childbirth (including vaginal delivery), and breastfeeding, the chance of perinatal transmission is less than 1%.
Some options for reducing the chance of perinatal transmission for those who are not virally suppressed include planning a cesarean delivery (also called a C-section) and using formula instead of breastfeeding.
All babies exposed to HIV during birth should receive HIV medicines, preferably within six hours of delivery.
To learn more, read the HIVinfo fact sheets Preventing Perinatal Transmission of HIV During Pregnancy and Childbirth and Preventing Perinatal Transmission of HIV After Birth.
What happens if a child gets HIV?
ART is recommended for everyone with HIV, including children. These medicines help people with HIV live long, healthy lives and reduce the risk of HIV transmission.
Healthcare providers consider several factors when prescribing HIV treatment in children, including a child’s growth and development. For example, because children grow at different rates, the recommended dose of an HIV medicine may depend on a child’s weight rather than their age. Children who are unable to swallow a pill may take HIV medicines that come in liquid or powder form.
HIV treatment must be taken exactly as prescribed and, while the treatment regimen may change, it must be continued for life to control the virus. For many children, taking HIV medicines exactly as prescribed (called medication adherence) can be difficult.
Why can medication adherence be difficult for children?
Several factors can make medication adherence difficult for children with HIV. Examples of factors that can affect medication adherence in children include—
- A busy family schedule that makes it hard to take HIV medicine on time every day.
- Side effects from HIV medicines.
- Refusal to take medicine because it tastes unpleasant.
- Social barriers outside of the family’s control such as unstable housing, lack of transportation, or cost of the medication.
- A child’s age and developmental stage.
The HIVinfo fact sheet Following an HIV Treatment Regimen: Steps to Take Before and After Starting HIV Medicines includes tips on adherence. Some of the tips may be useful to children with HIV and their parents or caregivers.
What other challenges do children with HIV face?
Children with HIV may face challenges beyond taking their medicines, including:
- Managing ongoing health care needs: Attending regular doctor visits, lab tests, and vaccinations to support growth and treatment.
- Coping with emotional and social concerns: Handling worries about stigma, privacy, or feeling different from friends and family members.
- Navigating school and social life: Balancing health needs while staying active in school, sports, and friendships.
- Accessing support: Finding trusted adults, community programs, or HIV support groups (such as the Dandelions movement) that offer connection and encouragement.
With modern HIV treatment, children can look forward to long, healthy lives. Strong support systems and community resources can help them overcome certain challenges related to HIV. See the HIVinfo Community Resources for People With HIV fact sheet for more information on available resources.
This fact sheet is based on information from the following sources:
From CDC:
From the HIV Clinical Practice Guidelines at Clinicalinfo.HIV.gov:
- Guidelines for the Use of Antiretroviral Agents in Pediatric HIV Infection:
- Recommendations for the Use of Antiretroviral Drugs During Pregnancy and Interventions to Reduce Perinatal HIV Transmission in the United States:
Also see the HIV Source collection of HIV information and resources.
